How do I buy or sell a medical practice in Texas?
The acquisition or sale of a medical practice represents one of the most significant transactions in a physician’s career. In Texas, these transactions require careful navigation of complex legal, regulatory, and business considerations. This guide provides an overview of the essential elements parties must understand when buying or selling a medical practice, with particular attention to Texas-specific requirements and common pitfalls to avoid.
For a more in-depth discussion on the introductory steps to a transaction (LOI, Term Sheet, etc.), the valuation process (calculation and structuring of a transaction’s purchase price), and standard provisions in M&A transaction agreements, please see our article, What do I need to know before I buy or sell a business? .
Structuring the Transaction
Base Case for Medical Buyers: Asset Sale
Direct physician-to-physician sales of medical practices in Texas are typically structured as asset sales. Buyers prefer asset sales because they can “cherry-pick” the assets they want (e.g., medical equipment, patient lists, goodwill) and avoid inheriting liabilities such as malpractice claims or contractual obligations. Asset sales also allow for a step-up in the tax basis of acquired assets, which can provide future tax benefits for the buyer. Sellers typically prefer stock sales, as they are not as complex (e.g., stock transactions do not require as many third-party consents) and they typically provide capital gains treatment on the entire sales price if the practice is structured as a corporation for federal income tax purposes. In an asset sale (including any deemed asset sale for tax purposes), a portion of the proceeds will likely be taxed at ordinary rates due to depreciation recapture. However, sellers can strategically allocate more of the purchase price to assets taxed at capital gains rates (e.g., intangible assets, goodwill) to optimize the tax treatment of the transaction.
Additionally, in Texas, certain licenses, permits, and provider numbers may be tied to the corporate entity. However, a transfer of or change in ownership often requires reapplication for these numbers regardless of transaction structure.
Texas Corporate Practice of Medicine Doctrine and Impact on Structure for Non-Medical Buyers
Texas law prohibits corporations, non-physicians, and non-medical entities from practicing medicine, employing physicians to provide medical services, or make clinical decisions. This is known as the corporate practice of medicine (CPOM) doctrine. The CPOM doctrine exists to ensure that medical decisions are made for clinical, not financial, reasons. As a result, a medical practice must be owned and operated by licensed healthcare professionals (such as physicians, dentists, or other licensed providers).
This means a private equity firm, a general corporation, or a non-physician investor cannot simply buy the stock of the practice or the assets of the practice. Instead, the buyer must acquire the non-medical assets (e.g., real estate, office furniture, administrative contracts), while the medical practice itself must remain under the ownership and control of licensed professionals. The practice retains the right to practice medicine and employ physicians.
Management Service Organization and Friendly Physician Model
The management services organization (MSO) model provides a common workaround for non-medical buyers. To achieve this structure, the investor forms an MSO to purchase the practice’s non-clinical assets and enters into a management services agreement with the practice. Under this arrangement, the MSO provides administrative, operational, and financial support to the practice, but does not own or control the medical practice. After closing, the practice remains owned by a “Friendly Physician” (i.e., the selling physician and/or a new physician appointed by the buyer) and continues to provide medical services, while the MSO manages the business side of the practice. This structure allows non-medical entities to participate in the financial success of the practice without violating the CPOM doctrine.
Hospital Acquisitions
Hospitals, which are typically licensed healthcare entities (whether nonprofit or system-owned), can acquire medical practices either through asset purchases or merger transactions, depending on strategic and regulatory considerations. In an asset deal, the hospital purchases all of the practice’s assets (i.e., both clinical and non-clinical assets) and employs the selling physician directly. Post-closing, the hospital will assume full clinical and business control and integrate the practice into broader health delivery systems, including shared electronic health records, centralized billing, and coordinated care networks.
From the seller’s perspective, selling to a hospital can offer benefits such as stable employment opportunities for physicians, access to hospital resources, and potential transaction terms influenced by regulatory oversight and competitive dynamics. However, the physician will transition from being an owner to an employee or contractor for the hospital.
Valuing the Practice and Determining the Purchase Price
The purchase price and payment structure for a medical practice sale should be negotiated based on the value of the business, risk allocation, deal structure, and the financial needs and preferences of both buyer and seller. The parties should agree on a valuation method and payment terms, as well as any earnouts or contingent payments and holdbacks or escrows for potential indemnification claims or post-closing liabilities.
The federal Anti-Kickback Statute (AKS), which prohibits the exchange of anything of value to induce or reward referrals for services or products covered by federal healthcare programs, significantly influences the structuring of the purchase price in medical practice sales. The parties must ensure that the transaction does not constitute an illegal inducement for referrals or generate federal healthcare program business improperly. The following items must be considered when valuing the practice and structuring the purchase price for the transaction:
Fair Market Value (FMV) Requirement: Purchase price and any related compensation must be at or very close to fair market value for bona fide services or assets. Payment above FMV can be construed as a kickback or inducement to generate referrals, which violates AKS. Sellers and buyers must often obtain independent valuations to justify price amounts and payment terms under AKS safe harbors.
Avoidance of Volume or Value-Based Payments: The price or compensation structure cannot depend on the volume or value of referrals or business generated by the seller post-closing. For example, contingent payments based on the number of patients referred could trigger AKS liability, unless carefully carved out or fitting a safe harbor.
Earnouts and Contingent Considerations: While earnouts are common to bridge valuation gaps, they must be structured with caution so they do not constitute illegal remuneration tied to referrals or utilization. Structuring earnouts based on overall practice profitability or other non-referral-based metrics is safer and more defensible under AKS.
Documentation and Transparency: Agreements must clearly document the basis for price, payment schedules, and the lack of referral inducements. Transparent contractual language helps demonstrate compliance with AKS and protects parties if scrutinized by regulators.
Use of Safe Harbors: Structuring the deal within recognized AKS safe harbors—such as bona fide employment, personal services, or FMV leases and purchases—help shield payments from AKS risk and support lawful transactions.
Preparing for and Conducting Due Diligence
Key considerations during the diligence phase for the sale of a medical practice in Texas include a combination of legal, financial, regulatory, operational, and clinical matters to ensure a comprehensive evaluation and smooth transaction.
Legal and Regulatory Diligence
Confirm compliance with Texas corporate practice of medicine rules.
Verify professional entity status.
Texas law requires licensed professionals (including physicians) to provide professional services authorized by the Texas Business Organizations Code and relevant professional licensing boards. The most common entity forms for medical practices are Professional Associations (PAs) and Professional Limited Liability Companies (PLLCs), which restrict ownership and control to licensed professionals and ensure compliance with Texas professional regulation and CPOM rules.
Verify compliance with licensing requirements, including that all necessary professional licenses (physicians, PAs, RNs) are current and in good standing.
Review contracts including leases, vendor agreements, third-party payor contracts, and any existing management services agreements related to clinical and non-clinical services.
Assess any ongoing or potential regulatory investigations, malpractice claims, or compliance issues that could affect valuation or liability.
Financial and Tax Diligence
Analyze historical and current financial statements for revenue streams (patient collections, payer mix), expenses, accounts receivable aged reports, and potential write-offs.
Examine tax filings and implications of the sale type (asset vs. stock), including any built-in gains, depreciation recapture, and pass-through tax issues related to S-corporations or partnerships.
Evaluate the condition and ownership of tangible assets, equipment, and intellectual property included in the sale, along with proper titling and maintenance records.
Review lease agreements for required landlord approval for assignment on sale and any specific provisions restricting property use for medical practice.
Operational and Clinical Diligence
Review staffing structures, physician employment agreements, restrictive covenants, and non-compete clauses that may impact continuity or transition.
Investigate clinical operations, including patient volumes, referral patterns, quality metrics, and any contractual obligations with hospitals or health systems.
Review inventory technology systems in use (EHR, billing, practice management software) and determine if licenses or access transfer with the assets.
Ensure ongoing compliance with state healthcare laws, patient privacy rules (Texas Medical Privacy Act, aligned with HIPAA), and billing regulations, including Medicaid fraud prevention rules.
Evaluate state insurance requirements and claims history, including tail coverage and transition of coverage in case of sale of practice.
Transaction and Transition Planning
Assess timing and structure of the deal to ensure compliance with CPOM restrictions, particularly if involving MSO and friendly PC models or hospital acquisitions.
Plan for the post-closing integration of the practice operations, billing, and clinical oversight, including transition services agreements.
Examine any escrow, holdback, or indemnification provisions to mitigate post-closing risks.
Reviewing Compliance with Federal Regulations
The Stark Law and the Anti-Kickback Statute are key federal healthcare regulations designed to prevent financial conflicts of interest that could influence medical decision-making and patient referrals improperly. Diligencing a medical practice for compliance with these regulations is a critical part of the diligence process in any healthcare transaction due to the severe penalties for violations.
Stark Law
Prohibits physicians from referring Medicare or Medicaid patients to entities for certain “designated health services” (including radiology, lab work, physical therapy, and durable medical equipment) if the physician or their immediate family has a financial relationship with that entity, unless a specific exception applies.
The Stark Law is a strict liability statute, which means that intent to violate the law is not necessary for penalties. Violations can lead to denial of payment, refund of amounts collected, civil penalties, and exclusion from federal healthcare programs.
Diligence considerations
Review referral relationships: Identify all existing referral relationships between the medical practice and any entities (e.g., laboratories, imaging centers, hospitals) to ensure no improper referrals if the practice has financial relationship with these entities. Analyze all financial arrangements, leases, compensation agreements, and ownership interests.
Examine Written Agreements: Confirm that physician compensation arrangements comply with Stark Law exceptions, such as fair market value compensation for bona fide services and no volume or value-based remuneration. Validate terms on remuneration, service descriptions, duration, and termination clauses.
Check Disclosure and Reporting: Ensure timely and accurate reporting of financial relationships to Centers for Medicare & Medicaid Services (CMS) as required. Verify that no undisclosed ownership or compensation arrangements exist that could trigger Stark Law sanctions.
Anti-Kickback Statute
Prohibits anyone (i.e., not just physicians) from knowingly and willfully offering, paying, soliciting, or receiving remuneration to induce or reward referrals or generate federal healthcare program business.
The AKS is a criminal statute and requires proof of intent to commit fraud. Violations can result in fines, imprisonment, and/or exclusion from federal healthcare programs.
Diligence considerations
Audit Compensation and Business Arrangements: Review all compensation and business arrangements with referral sources or potential referral sources to detect any improper inducements, including payments, gifts, rebates, or benefits that could be viewed as intended to induce referrals of federal healthcare program patients. Evaluate if these arrangements satisfy AKS safe harbors or exceptions.
Assess Financial Incentives: Verify that compensation is consistent with fair market value and commercially reasonable. Ensure no disguised remuneration exists to influence referrals or generate business improperly.
Internal Policies and Training: Review documentation regarding the practice’s compliance program, including policies, training, and audits designed to prevent AKS violations and promote adherence to federal and state anti-kickback rules.
Drafting Transaction Documents
Sales of medical practices involve significantly more regulatory complexity and specialized documentation than typical commercial M&A transactions. The healthcare industry's unique regulatory framework (including the CPOM doctrine, Stark Law, AKS, HIPAA, and state licensing requirements) necessitates additional legal, compliance, and operational considerations that do not typically appear in standard business acquisitions.
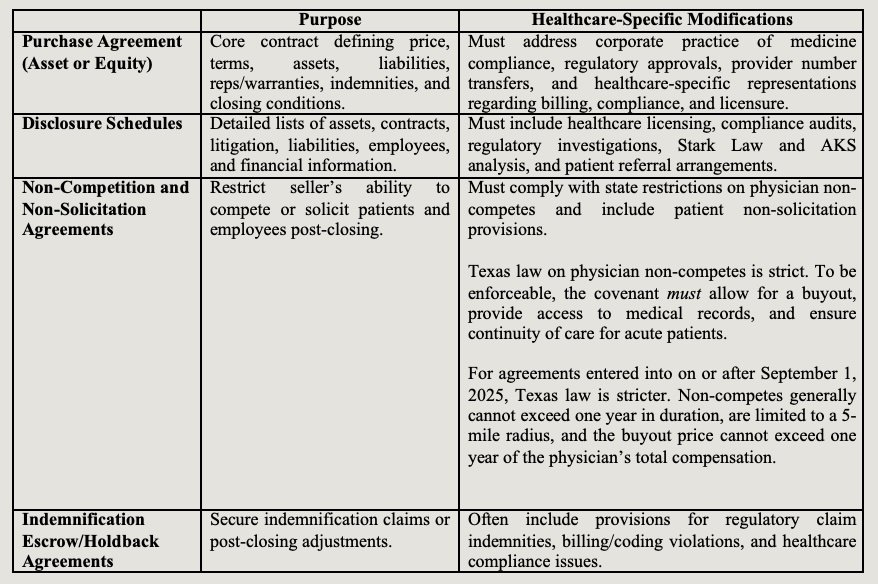
Core Transaction Documents
Additional Documents Unique to Medical Practice Transactions
Management Services Agreement (MSA)
When the buyer is a non-medical entity (e.g., private equity, MSO, or non-licensed company) in states with CPOM doctrines, the MSA will split the business into two distinct parts to comply with the CPOM restrictions and govern the relationship between the physician-owned medical practice and the non-physician investor or MSO. The MSA should specify that the practice will retain 100% control over all clinical decisions, while the MSO will handle all non-clinical business operations in exchange for a management fee.
Key Provisions:
Explicit provisions that the MSO has zero control over medical decisions and that the physician retains autonomy over all patient care protocols, medical decision-making, hiring and supervision of clinical staff (e.g., nurses, PAs), and professional credentialing decisions.
Specify non-clinical services to be provided by the MSO (e.g., billing and collections, human resources and payroll, IT services and support, facility management, marketing, accounting).
Specify the management fee to be received by the MSO.
In many states, MSOs charge a percentage of the practice’s revenue (e.g., 30% of collections). However, in Texas, percentage-based management fees are high-risk and often viewed by the Texas Medical Board as illegal fee-splitting. Instead, fees are typically structured as flat monthly fees representing the fair market value of the services provided by the MSO. Fees can be revised annually but should not fluctuate month-to-month based on patient volume.
Specify term, renewal, and termination rights.
Stock Restriction and Equity Alignment Agreement
In the “friendly physician” structure, the non-medical investors control the MSO, while the physicians nominally own the practice. These documents ensure that the non-medical investors have economic control and governance rights of the practice, without actual legal ownership.
Key Provisions:
Restrictions on transfer of physician ownership shares.
Consent rights for major decisions (employment of new physicians, contract termination, location changes).
Buy-sell provisions favoring the MSO.
Equity transfer obligations if physician leaves or loses licensure.
Veto rights on certain governance matters.
Physician Employment or Transition Agreement
This agreement defines post-closing employment terms, compensation, duties, restrictive covenants, and termination rights of the selling physician. Employment agreements in standard M&A are common but are typically less complex. Agreements in healthcare transactions must carefully document fair market value compensation and compliance with federal fraud and abuse statutes.
Key Provisions:
Compensation structure (salary, productivity bonuses, equity interests if applicable).
Malpractice tail insurance obligations and coverage.
Restrictive covenants (non-compete, non-solicit, non-disparagement).
Credentialing and privileging responsibilities.
Termination and change-of-control provisions.
Compliance with anti-kickback and Stark Law exceptions for bona fide employment.
Transition Documents
Transition documents facilitate the smooth handoff of operations from seller to buyer post-closing.
Patient Records Custodianship/Transfer Agreement: Required under HIPAA and Texas Health and Safety Code to document proper custody, access, and retention of patient medical records. Must comply with state record retention requirements (typically 6-7+ years minimum).
Payer/Insurance Notifications and Re-Credentialing: Required by Centers for Medicare & Medicaid Services (CMS), state medical boards, and payers to maintain active provider enrollment and billing privileges post-closing. Failure to notify can result in claim denials and loss of provider status.
Lease Assignment and Landlord Acknowledgment: Legally required if the practice operates on leased premises; assignment without landlord consent may constitute breach of lease and give landlord grounds to terminate.
Hospital Privileges/Credentialing Notice: Required if physicians maintain hospital staff appointments; must notify hospital medical staff of ownership/employment changes to maintain privileges.
Employee Transition/Retention Agreements: If the purchase agreement specifies retained employees or retention bonuses, formal employment or retention agreements must be executed at closing to be enforceable.
Accounts Receivable Collection Agreement: If the purchase agreement addresses receivables (seller retains, buyer collects, or profit-sharing), a formal collection and banking agreement is needed to document the arrangement and avoid disputes.
The sale or acquisition of a medical practice represents one of the most significant financial and operational transactions a healthcare professional or healthcare company will undertake. The convergence of complex healthcare regulations, tax considerations, employment law, and operational integration requirements demands specialized legal expertise and careful planning.
Whether you are a physician selling your practice, a healthcare entrepreneur acquiring practices for a platform or roll-up strategy, or a private equity firm investing in healthcare, the transaction's success depends on engaging experienced healthcare legal counsel early in the process. A skilled healthcare attorney will help structure the transaction for regulatory compliance, conduct thorough due diligence to identify and mitigate risks, draft comprehensive transaction documents that protect your interests, and facilitate a smooth post-closing transition.
Ready to start? Click here to schedule a consultation with Kalaria Law today and discuss your specific goals in buying or selling a medical practice, while navigating the regulatory landscape.
Disclaimer: This article is for general informational purposes only and does not constitute formal legal advice.